AHP Signs
& Symptoms
KNOW WHEN TO
SUSPECT AHP*
Severe, Diffuse
Abdominal Pain1,2
+
1 Or More Of The Following
AUTONOMICNervous System1,2
- Nausea/vomiting
- Constipation
- Tachycardia
- Systemic arterial hypertension
CENTRALNervous System1-3
- Seizures
- Anxiety
- Mental status changes
PERIPHERALNervous System1,2
- Limb weakness or pain
- Peripheral neuropathy
cutaneous2
- Skin lesions on sun-exposed skin (Cutaneous symptoms primarily occur in HCP and VP)
OTHERCommon AHP Symptoms2,4
- Hyponatremia
- Dark, reddish urine
*There are 4 types of AHP. Over 80% of cases are acute intermittent porphyria (AIP), followed by variegate porphyria (VP), hereditary coproporphyria (HCP), and the extremely rare ALAD-deficiency porphyria (ADP).2,5,6
AHP FEATURES A
BROAD RANGE OF SYMPTOMS†
In addition to severe, diffuse abdominal pain without fever or leukocytosis, other common symptoms of AHP include nausea and vomiting, limb weakness or pain, anxiety, confusion, and skin lesions on sun-exposed areas (HCP and VP primarily). Tachycardia and hyponatremia are often present in acute attacks of AHP.2,3,6
These symptoms reflect neurotoxic effects across the autonomic, peripheral, and central nervous systems. Patients may experience one characteristic symptom or multiple symptoms that may lead to a diagnosis2,3:

-
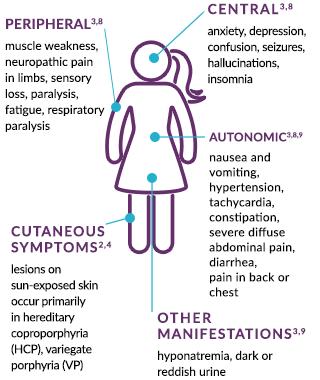
Central3,8
anxiety, depression, confusion, seizures, hallucinations, insomnia
-
Peripheral3,8
muscle weakness, neuropathic pain in limbs, sensory loss, paralysis, fatigue, respiratory paralysis
-
Autonomic3,8,9
nausea and vomiting, hypertension, tachycardia, constipation, severe diffuse abdominal pain, diarrhea, pain in back or chest
-
Cutaneous symptoms2,4
lesions on sun-exposed skin occur primarily in hereditary coproporphyria (HCP) and variegate porphyria (VP)
-
Other Manifestations3,9
hyponatremia, dark or reddish urine
†These are not all the possible symptoms of AHP.
As healthcare providers working with porphyria patients, it’s critical that we remember many are suffering from mentally-imparting brain fog. The brain fog is a warning signal of a beginning attack and makes the caregiver’s role so critical.
R. J. Desnick, MD, PhDDean for Genetics and Genomic Medicine, Icahn School of Medicine at Mount Sinai
Acute attacks in genetically predisposed patients are frequently preceded by environmental or hormonal triggers.2,4,9,10
Some known triggers of acute attacks include2,4,9,10:
The use of some medications in the following drug classes‡:
- Anesthetics
- Oral contraceptives
- Anticonvulsants
- Antihistamines
- Antihyperglycemics
- Antimicrobials
- Hormones
- Migraine drugs
- Sedatives
Hormonal fluctuations during the menstrual cycle§
Extreme dieting
Excessive alcohol consumption
Smoking
Stress caused by:
- Infections
- Surgery
- Physical exhaustion
- Psychological stress
‡You may access the American Porphyria Foundation to learn more about the potential of certain medications to trigger an attack: https://porphyriafoundation.org/drugdatabase. This database is developed and maintained by the American Porphyria Foundation. Alnylam Pharmaceuticals does not endorse and is not responsible for the content on the sites that are not owned and operated by Alnylam.
§Hormones are at their highest fluctuation 2 weeks before a woman's menstrual cycle begins.
AHP can be chronic with progressive elements11-15
In a large natural history study of patients with recurrent attacks,‖ 65% of patients reported chronic symptoms in between attacks (including pain), and 46% reported experiencing symptoms every day.
‖Recurrent attacks in EXPLORE were defined as ≥3 attacks within 12 months or prophylactic use of hemin or GnRH analog.
LONG-TERM COMPLICATIONS ASSOCIATED
WITH AHP
Long-term complications of AHP may include chronic hypertension, chronic kidney disease, hepatocellular carcinoma, and psychological problems.
An important goal in the management of AHP is to help prevent irreversible long-term damage.
Patients with AHP may have an increased risk of suicide related to comorbidities of psychiatric symptoms and chronic pain.16
AHP is often misdiagnosed
due to nonspecific symptoms
The signs and symptoms of AHP can mimic those of numerous common diseases, such as irritable bowel syndrome, endometriosis, fibromyalgia, and psychiatric disorders. These similarities can lead to misdiagnoses.1,17,18
In a retrospective review of 546 charts of patients with AHP submitted by 175 healthcare providers from the US, EU, Canada, and Japan, 26% of patients with AHP were initially misdiagnosed.17
Be Aware of Similar Symptoms1,17,18




DELAYED DIAGNOSIS CAN BURDEN PATIENTS' HEALTH AND LONG-TERM WELL-BEING2,6,9,11,19,20

Delayed diagnosis and misdiagnoses can lead to unnecessary procedures. The symptoms of AHP often resemble those of other diseases in the gastrointestinal, gynecological, and neurological or neuropsychiatric areas. Severe symptoms can lead to hospitalizations and unnecessary procedures. Misdiagnosis is common, and people with AHP can wait years for an accurate and confirmed diagnosis. Patients with recurrent attacks of AHP had a mean of 82 days (range: 10 to 374) of hospitalization over a mean observation time of 21 years.1,2,11,17-19,21,22
Acute hepatic porphyrias put deep strain on family relationships. Patients often miss family outings, can’t help with chores or contribute financially, and often feel like a burden to their loved ones, adding emotional pain to the physical.
Karl E. Anderson, MD FACP Professor, Departments of Preventive Medicine and Community Health, and Internal Medicine (Division of Gastroenterology), University of Texas Medical Branch
AHP Reduces Quality of Life (QoL)
AHP is a debilitating disease with a significant impact on patients’ daily lives and social functioning, both during and in between attacks. In a study of patients with AIP (the most common type of AHP) with recurrent acute attacks, 63% reported a negative impact on relationships or social roles, 74% reported interference with walking, and 84% reported impaired ability to work.5

¶As reported in a population with acute intermittent porphyria with multiple attacks (3 or more) within the last year.5
Long-term chronic pain, emotional stress, comorbid depression and anxiety, and fear of unpredictable attacks contribute to a lower QoL for some patients with AHP.5,23,24
See How Porphyria Impacts the Lives of Real Patients
Watch the video below to see how acute intermittent porphyria (AIP) has affected 3 generations of women with severe attacks.
References: 1. Ventura P, Cappellini MD, Biolcati G, Guida CC, Rocchi E; Gruppo Italiano Porfiria (GrIP). Eur J Intern Med. 2014;25(6):497-505. 2. Anderson KE, Bloomer JR, Bonkovsky HL, et al. Ann Intern Med. 2005;142(6):439-450. 3. Puy H, Gouya L, Deybach JC. Lancet. 2010;375(9718):924-937. 4. Balwani M, Wang B, Anderson KE, et al; Porphyrias Consortium of the Rare Diseases Clinical Research Network. Hepatology. 2017;66(4):1314-1322. 5. Simon A, Pompilus F, Querbes W, et al. Patient. 2018;11(5):527-537. 6. Bissell DM, Wang B. J Clin Transl Hepatol. 2015;3(1):17-26. 7. Gouya L, Bloomer JR, Balwani M, et al. Presented at: 2017 International Congress on Porphyrins and Porphyrias; June 26, 2017; Bordeaux, France. 8. Harper P, Sardh E. Expert Opin Orphan Drugs. 2014;2(4):349-368. 9. Bissell DM, Anderson KE, Bonkovsky HL. N Engl J Med. 2017;377(9):862-872. 10. Whatley SD, Badminton MN. In: Adam MP, Ardinger HH, Pagon RA, et al, eds.